Contemplating a Caribbean vacation to escape Whistler's uninspiring winter? You might want to add a crash course on chikungunya (chicken-goon-ya) to that list of pre-trip preparations.
Despite its sonic allusion to a gustatory gumbo, chikungunya is neither an island dish nor an emerging regional foodie trend; it is, however, a recipe for disaster penned by the one-two-three combination of rapid globalization, climate change and invasive species.
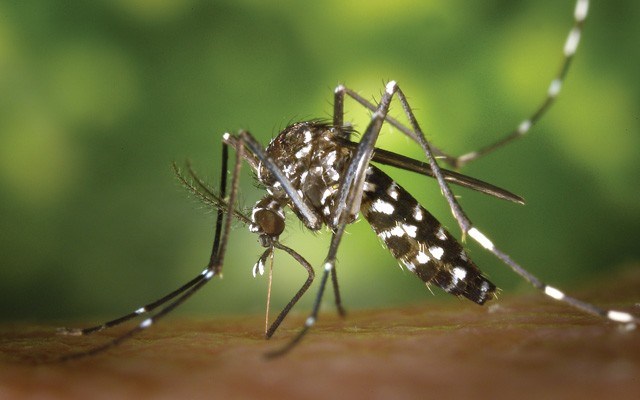
A virus endemic to southeast Asia and sub-Saharan Africa, chikungunya is yet another in the litany of mosquito-borne diseases to jump oceans in recent years. The name derives from the Makonde language of southern Tanzania (where the disease was discovered in 1955), and means "that which bends up," graphic reference to the cringing pain it causes. Chikungunya attacks the joints, bringing fever, headache and arthritis-like symptoms. It generally lasts only a few days, but in some cases the joint pain can persist for months. There's no cure, no vaccine, no treatment, though fatalities are thankfully rare, according to the U.S. Centers for Disease Control (CDC). Once infected you'll have lifelong immunity to the disease, but the only way to actually prevent it is to avoid its natural vectors — mosquitoes of the genus Aedes. Back when the African yellow fever mosquito (Aedes aegypti) and Asian tiger mosquito (Ae. albopictus) were found only in parts of tropical Asia and Africa, avoidance on this side of the pond was easy. These days, not so much.
In 2006 an outbreak of chikungunya in India infected over a million people. One of those humans hopped on a plane and brought the virus to Italy where the Asian tiger mosquito had previously been introduced; with a ready-and-waiting reservoir/vector, 200 more subsequently fell ill. Further outbreaks on Pacific and Indian Ocean Islands, and in southern France likewise relied on prior establishment of non-native Aedes invaders — variously transported via the international used tire and ornamental plant trades. With Dengue fever (also transmitted by Aedes) on the rise as well, global health researchers had long predicted chikungunya to eventually show up wherever Aedes mosquitoes gained a foothold. As one of the World's 100 Worst Invaders, and with a broader tolerance of temperate climates than its African counterpart, this means pretty much everywhere for the Asian tiger mosquito — including, BTW, the Pacific Northwest.
Before Christmas I'd spoken with invasive species researcher Dr. Anthony Ricciardi of McGill University in Montreal about a recent book that painted much of the growing field of invasion science as institutionalized exaggeration in which overblown priorities were churned out by sky-is-falling doomsayers and their lap-dog funding agencies. "That's nonsense. Everything is exaggerated in the media these days," Ricciardi told me, "everything — but we all know that. Storms are hyped up but we don't ignore the fact that they're occurring. Exaggeration doesn't make the original information less important."
In other words, it would be at our peril to ignore the increasingly strident warnings of 1,500 International Panel on Climate Change scientists simply because of the media's affection for only the direst predictions. We'd be similarly crazy, Ricciardi reasons, to ignore the enormous number of respected researchers pointing to potential invasive species problems. "Here's an example: the Asian tiger mosquito vectors all sorts of diseases, and it's all over North America now. Maybe the diseases haven't arrived, but the mosquito's presence is a disaster waiting to happen."
Prescient. Only two weeks later, the CDC was warning sun-seekers up and down the eastern seaboard of the burgeoning chikungunya outbreak. Only a year earlier, on Dec.6, 2013, the World Health Organization reported the first case of local transmission of chikungunya on Saint Martin. That is, the island's mosquitoes were infected and now passing it to people — the first time this was reported in the Americas. How fast could chikungunya spread across a 2,750,000 km2 archipelago? Well, how well distributed were its invasive mosquito vectors?
Apparently exceptionally well. Only ten months later, on Oct. 21, 2014, the CDC was reporting local transmission on 25 Caribbean islands, French Guyana in South America and, of course, Florida, North America's welcome mat for all tropical interlopers.
None of this was news to Dr. Isaac Bogoch, Assistant Professor in the Department of Medicine at the University of Toronto and a tropical disease specialist at Toronto General Hospital. In June 2014, Bogoch was a co-author on "Assessing the Origin of and Potential for International Spread of Chikungunya Virus from the Caribbean," in the online journal PLoS Currents, which specializes in the rapid sharing of research in progress. Using airline arrival/departure information between the Caribbean and other parts of the world, Bogoch and fellow researchers constructed a predictive model explaining the likely origin and potential spread of the current outbreak. Their results were spot on.
"We've been tracking and modeling different emerging and re-emerging infectious diseases," Bogoch explains. "These are influenced by human migration patterns, socioeconomic patterns, agricultural patterns, and climate and ecological change. Globalization and accelerated rates of air travel are the root of the problems we're seeing — and anticipating."In other words, international travel by infected persons and the "increasing geographic availability of competent vectors" — Bogoch's polite way of framing invasive species — set the stage for chikungunya's introduction and spread in the Americas. Add that to an increase in appropriate environmental factors for both vector and virus (e.g., an average temperature above 20C), and it equals over 16,000 confirmed and 900,000 suspected cases of chikungunya as of January 2015.
"Much has been written lately about the expansion of various animals' ranges being coincident with the spread of certain diseases beyond their traditional geographic areas," notes Bogoch. "For instance, why are Ixodes ticks (which carry the Borrelia bacterium responsible for Lyme disease) expanding their range? Because of the movements of birds, rodents and deer in response to climate change."
The takeaway on chikungunya from a public health standpoint? "Basically there's a new kid on the block of mosquito-borne diseases like malaria, Dengue fever, encephalitis and West Nile virus. West Nile has been endemic in North America for decades now. Every summer it flares up, some years worse than others, but it's here to stay. Chikungunya is the latest but not the last."
As Bogoch summarizes, taking a 30,000-foot view of this trend we have to ask: What's going on? "The answer is obvious — globalization and mobility and interconnectivity and changing weather patterns — and none of those are going away either."
Leslie Anthony is a Whistler-based author, editor, biologist and bon vivant who has never met a mountain he didn't like.